Disclaimer: This article is not intended to offer medical advice, and anyone who has tested positive for COVID-19, or suspects they may have contracted the disease, should contact their doctor regarding care.
Summary
Beyond research into vaccines and traditional therapeutics, the medical community is exploring other ways of helping to prevent, and reduce, symptoms of COVID-19. One promising supplement is a common probiotic. In this article we will discuss the studies that have been conducted, their findings, and answer the question: who could benefit from taking probiotics?
We are fast approaching the second anniversary of the outbreak of the COVID-19 pandemic, and despite vaccines and booster shots, the new Omicron variant is fueling a surge in COVID-19 cases – causing some to dub January 2022, “Janvid.” The continued spread of the pandemic is bolstered by the height of flu season – people’s immunity is already lowered, and some people, unable to discern whether they have contracted the flu or COVID may accidentally infect others. In light of this, the medical community has been researching ways to help prevent and mitigate symptoms of COVID-19.
Probiotics for Prevention?
While the term ‘probiotics’ may conjure images of yogurt and kefir for the average person, these live microorganisms are known to boost immunity, and may offer an accessible way for people to help flatten the COVID-19 curve [Image 1]. While trials haven’t been conducted for the use of probiotics against COVID-19 yet, studies such as Olivares et al. (2007), have shown the potential antiviral impact of probiotics. Olivares et al., orally administered the probiotic strain Lactobacillus fermentum CECT5716 for two week prior to, and post, influenza vaccination. Compared to the placebo group, the probiotic group showed increased presence of antibodies, and stronger immune Th1 response.
About the Author: Alexandra Narin
Alexandra is a Content Marketing Specialist and Grant Writer for InVivo Biosystems. She graduated from the University of St Andrews in 2020 where she earned a Joint MA Honours Degree in English & Psychology/Neuroscience with BPS [British Psychology Society] Accreditation. She has worked as a research assistant, examining the LEC’s (lateral entorhinal cortex) involvement in spatial memory and integrating long term multimodal item-context associations, and completed her dissertation on how the number and kinds of sensory cues affect memory persistence across timescales. Her hobbies include running, boxing, and reading.
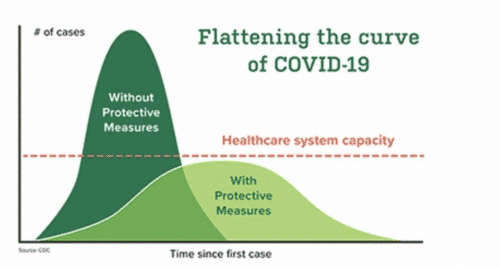
Image 1. Why preventing infection of COVID-19 is necessary (UAB, 2020).
Probiotics MoA: Why Probiotics could Help Mitigate COVID-19 Symptoms
Evidence of probiotics’ ability to affect coronaviruses is strengthened from the symptoms of COVID-19 patients – 74% to 86% of people hospitalized with COVID-19 develop gastrointestinal complications. Thus, ‘intestinal dysbiosis’ is recognized as one of the main side effects of the disease. As probiotics are known to help restore gut homeostasis, including a probiotic strain into the treatment regimen for critically ill patients could be beneficial without being overly expensive or invasive. Furthermore, there is growing evidence of the interconnectivity of human bodies in maintaining homeostasis (if there is dysbiosis in the gut, there is likely disruption in other systems on your body such as the brain and lungs). The gut-lung axis (GLA) can shape immune responses, and can interfere with the course of a respiratory disease (such as COVID-19).
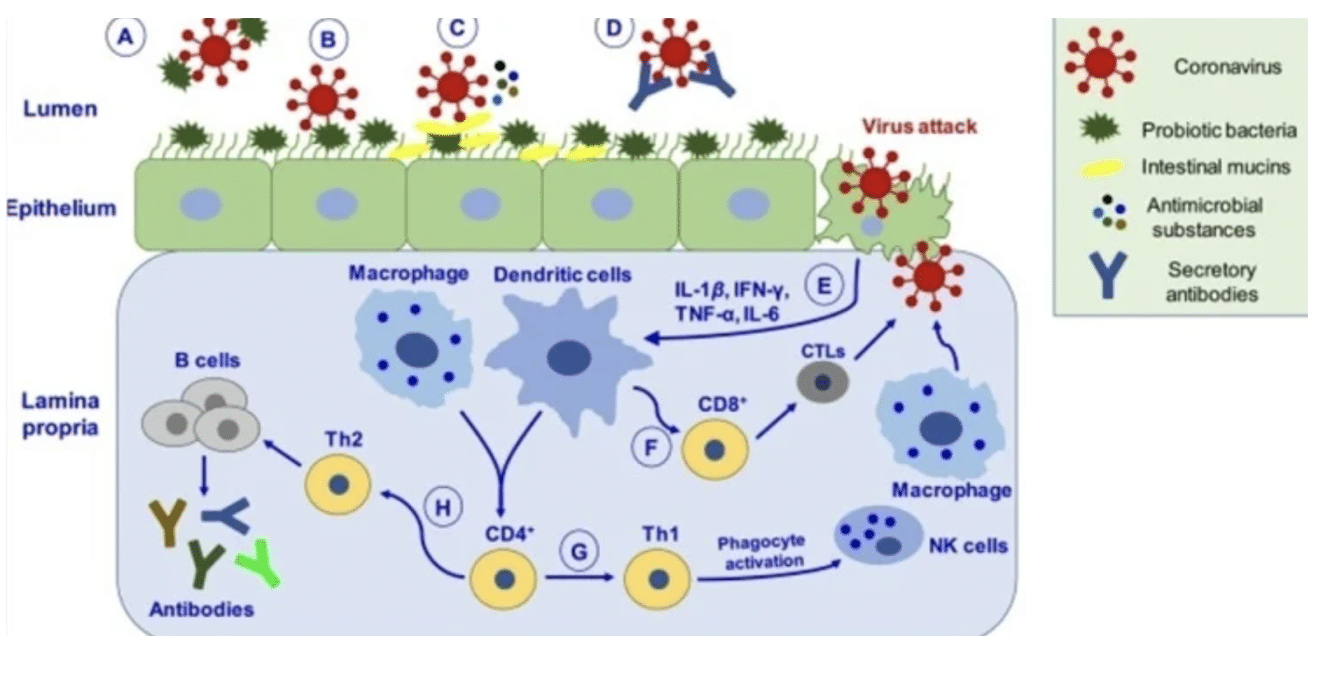
Image 2. Depiction of putative mechanisms by which probiotics may help manage coronavirus infection. ( A ) Probiotic bacteria can hinder the adsorption process via directly binding to the virus and inhibiting entry into epithelial cells. ( B ) Binding of probiotic bacteria to the epithelial surface can cause steric hindrance and block the virus’s attachment to the host cell receptor. ( C ) Probiotic bacteria releases antimicrobial substances (such as bacteriocins, biosurfactants, lactic acid, hydrogen peroxide, nitric oxide, organic acids) and intestinal mucins from mucosal cells, which can effectively inhibit virus proliferation. ( D ) Virus neutralized by secretory antibodies like IgA. ( E ) Upon virus attack in epithelial cells, probiotics mediate their antiviral effects by eliciting immune responses by activating macrophages and dendritic cells. ( F ) Activation of immune response leads to differentiating CD8 + T lymphocytes into CTLs, capable of destroying virus-infected cells. ( G ) CD4 + T lymphocytes cells differentiate into Th1, which activates phagocytosis through NK cells and macrophages, promoting pathogen killing. ( H ) CD4 + cells differentiate into Th2 cells, which induce B-cells’ proliferation that produces antibodies like IgA, IgG, and IgM. CTLs, cytotoxic T-lymphocytes; Th1, T-helper cells type 1 (Thomas, 2021).
Can Probiotics Offer Relief for COVID-19 Long-haulers?
Dr Siew Chien Ng, associate director of the Centre for Gut Microbiota Research at the Chinese University of Hong Kong (CUHK), led the research team that was the first in the world to report that the composition of gut microorganisms (microbiota) in COVID-19 patients greatly differs from the healthy population. Ng stressed the effect that the gut microbiota imbalance could have, stating that even once people are considered ‘recovered’ from COVID-19 they continue to have a high degree of abnormality in their gut microbiota, and that this could play a role in long-haul COVID-19. Similarly, a study out of Sweden found that patients who experienced long-haul symptoms (such as brain fog, muscle soreness and fatigue), reported that these lessened after 14 days of probiotic usage.
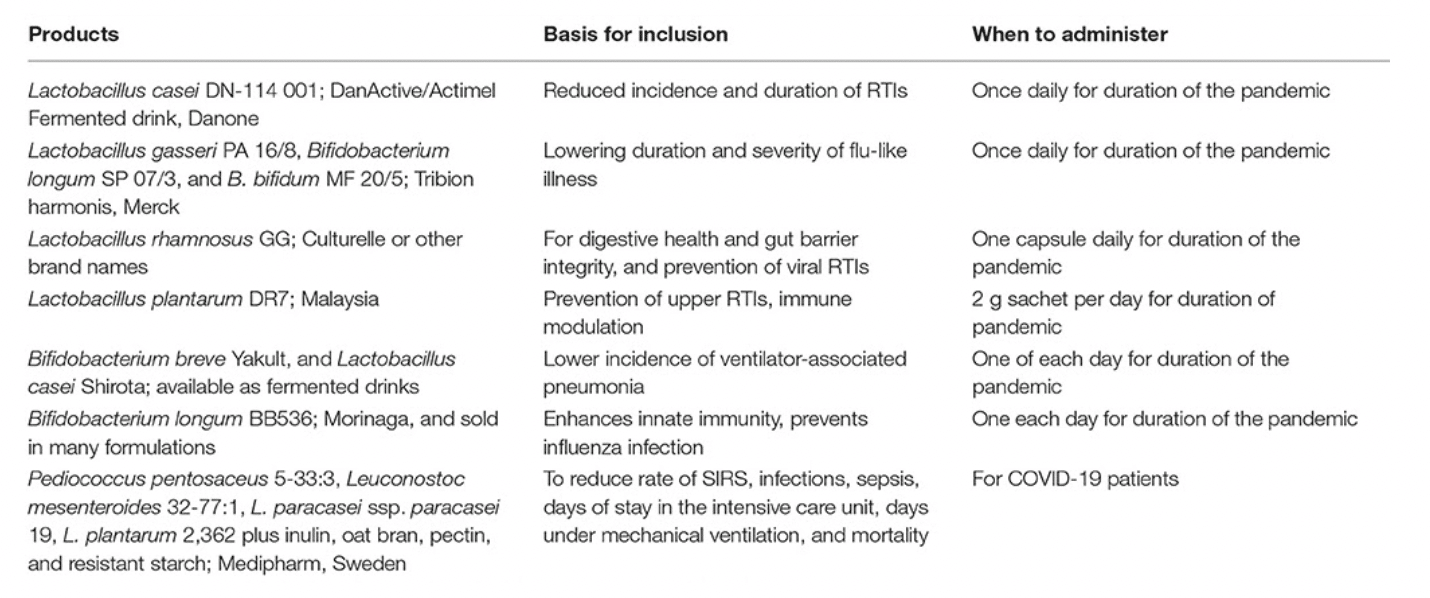
Image 3. Examples (not exclusive) of probiotic products with documentation in human studies that may have relevance to reducing the burden of the coronavirus pandemic (Baud et al., 2020).
Conclusion
As extensive studies have yet to be conducted on COVID-19 patients, currently there is no definitive answer as to whether probiotics help prevent or mitigate the disease, and if so – which probiotic strains in particular have the most impact. This being said, experts agree that there is no harm in adding a probiotic supplement into your routine.
To learn more about your gut, its impact on your health, and your microbiome check out our recent article: Modeling Gut Microbiome Effects in Alternative Animal Models – Finding the Happy Biota for a Long and Healthy Life here.
References:
- Baud D, Dimopoulou Agri V, Gibson GR, Reid G and Giannoni E (2020) Using Probiotics to Flatten the Curve of Coronavirus Disease COVID-2019 Pandemic. Front. Public Health 8:186. doi: 10.3389/fpubh.2020.00186
- Graf, N. (2021). Probiotics could help some COVID-19 long-hauler symptoms, abc15 Arizona. https://www.abc15.com/news/vaccine-in-arizona/probiotics-could-help-some-covid-19-long-hauler-symptoms
- Kaafarani, H., El Moheb, M., Hwabejire, J. O., Naar, L., Christensen, M. A., Breen, K., Gaitanidis, A., Alser, O., Mashbari, H., Bankhead-Kendall, B., Mokhtari, A., Maurer, L., Kapoen, C., Langeveld, K., El Hechi, M. W., Lee, J., Mendoza, A. E., Saillant, N. N., Parks, J., Fawley, J., … Velmahos, G. C. (2020). Gastrointestinal Complications in Critically Ill Patients With COVID-19. Annals of surgery, 272(2), e61-e62. https://doi.org/10.1097/SLA.0000000000004004
- Marazzato, M., Ceccarelli, G., & d’Ettorre, G. (2021). Dysbiosis in SARS-CoV-2-Infected Patients. Gastroenterology, 160(6), 2195. https://doi.org/10.1053/j.gastro.2020.12.056
- Sun, J. K., Liu, Y., Zou, L., Zhang, W. H., Li, J. J., Wang, Y., Kan, X. H., Chen, J. D., Shi, Q. K., & Yuan, S. T. (2020). Acute gastrointestinal injury in critically ill patients with COVID-19 in Wuhan, China. World journal of gastroenterology, 26(39), 6087-6097. https://doi.org/10.3748/wjg.v26.i39.6087
- Tomas, M., Capanoglu, E., Bahrami, A., Hosseini, H., Akbari-Alavijeh, S., Shaddel, R., Rehman, A., Rezaei, A., Rashidinejad, A., Garavand, F., Goudarzi, M., & Jafari, S. M. (2021). The direct and indirect effects of bioactive compounds against coronavirus. Food Frontiers, 1-28. https://doi.org/10.1002/fft2.119
- Thomas, Liji (2021). Probiotics may be beneficial in COVID-19 treatment. News, Medical Life Sciences. https://www.news-medical.net/news/20210217/Probiotics-may-be-beneficial-in-COVID-19-treatment.aspx
- UAB (2020). To stop spread of COVID-19, ‘flattening the curve’ is critical, The University of Alabama at Birmingham, https://www.uab.edu/news/health/item/11180-to-stop-spread-of-covid-19-flattening-the-curve-is-critical
- Yan, H. & Vera, A. (2021). January will be ‘a really, really hard month’ as the Omicron variant fuels spike in infections, expert says. CNN Website, https://www.cnn.com/2021/12/28/us/us-coronavirus-tuesday/index.html
- Enaud R, Prevel R, Ciarlo E, Beaufils F, Wieërs G, Guery B and Delhaes L (2020) The Gut-Lung Axis in Health and Respiratory Diseases: A Place for Inter-Organ and Inter-Kingdom Crosstalks. Front. Cell. Infect. Microbiol. 10:9. doi: 10.3389/fcimb.2020.00009