Summary:
The Western Medical Community has long viewed acupuncture with skepticism, but increasingly physicians are exploring the potential benefits of this traditional practice. In fact, despite often being referred to as a pseudoscience, recent research has found significant benefits of acupuncture treatment for patients with chronic pain and those suffering from opioid addiction. In this article we will discuss acupuncture — what it is, its history and applications, and how it is now being viewed as a potentially game-changing treatment to be used in conjunction with western pharmaceutical therapies.
Acupuncture is the Traditional Chinese Medicine (TCM) practice of inserting needles into particular pressure points to relieve pain, manage symptoms, or increase fertility. In my case, acupuncture was first recommended to me when I was seven as a way to manage scoliosis. At first, I was quite hesitant (most children do not enjoy the thought of being poked with needles), but after a few years it seemed worth a try. And I found what millions of people worldwide have experienced — it worked.
While acupuncture has historically been dismissed by the Western Medical Community — even Wikipedia’s current article on the topic stating that “Acupuncture is a pseudoscience; the theories and practices of TCM are not based on scientific knowledge, and it has been characterized as quackery” — increasingly, research is being conducted and finding evidence of its benefits on conditions ranging from headaches to chemotherapy management (Wikipedia, 2022).
Current State of Acupuncture as a Medical Therapy
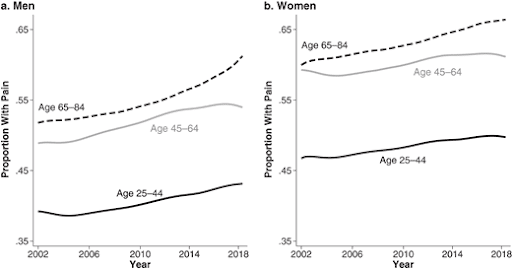
Figure 1. Pain trends 2002–2018 for U.S. adults ages 25–84 (Zajacova, Grol-Prokopczyk & Zimmer, 2021)
Acupuncture as a Reaction to the Opioid Crisis
In the late 1990s health care providers increasingly began prescribing opioids due to reassurance that opioids offered a non-addictive way to relieve pain. We now know that this is far from the truth, and while the tendency to misuse opioids is highly publicized, opioids are still being over prescribed leading to high rates of overdosing — in 2019 alone nearly 50,000 Americans died from an opioid-involved overdose (NIH, 2021). Chronic pain sufferers are particularly at risk for becoming addicted to opioids, as opioids are prescribed to over 1 in 5 (22.1%) patients with chronic pain (Dahlhamer et al., 2021). Chronic pain can take many forms, but some of the most common types are low back and neck pain, osteoarthritis, and headaches.
“8-12% of patients prescribed opioids for chronic pain misuse them” – NIH, 2021
“8-12% of patients prescribed opioids for chronic pain misuse them” – NIH, 2021
“8-12% of patients prescribed opioids for chronic pain misuse them” – NIH, 2021
So, there is the need and motivation to incorporate alternative pain relief treatments into Western medicine — how can acupuncture help? The types of pain that acupuncture is used for alleviating overlaps with the previously mentioned types of chronic pain (low back and neck pain, osteoarthritis, and headaches). Recently it was found that acupuncture could reduce the frequency of chronic tension headaches by 50%, and as these are the most common type of chronic headaches this finding provides a lot of support to acupuncture therapy (Searing, 2022). Acupuncture has also been shown to relieve pain and improve the quality of life for those suffering from Multiple Sclerosis and Fibromyalgia, with benefits such as: decreased fatigue, delayed disease progression, improved bladder function, and reduced spasms (Whelan, 2022; Schweiger et al., 2020).
These promising research findings have even been acknowledged by the Medicare system, which, in 2020 opted to nationally cover acupuncture for chronic back pain. In their announcement the Centers for Medicare and Medicaid Services specifically cited the safety of acupuncture compared to the consequences of potentially addictive narcotic painkillers as the rationale behind their decision to provide this coverage (Dooley Young, 2020).
The Difficulties with Researching Acupuncture’s Efficacy
While it may seem like acupuncture is a “no brainer”, there are notable challenges for acupuncture research as clinical trials often differ in the type and duration of treatments. The personalized aspect of acupuncture is one of the therapy’s greatest strengths, however, it also makes generalizations difficult. Furthermore, due to the stigma surrounding alternative medicines, there is concern that results of acupuncture treatments could be swayed based on personal opinion.
Future of Acupuncture in Western Medicine
The increased interest in acupuncture by the Western medical community is reflected by the growing popularity of TCM practices, such as herbalism, in the broader USA commercial market.
Over the last two decades nutraceuticals have become a booming industry, with companies such as NOOCI, Mount Lai, and Elix, even finding success marketing to a younger (millenial and Gen Z) audience. We at InVivo have noticed this shift as well and recently announced our collaboration with Chenland Nutraceuticals to test the efficacy of their TCM-based longevity formulation.
Overall, the increased usage of alternative therapies such as acupuncture presents an exciting future for medicine — allowing clinicians to decrease the amount of pharmaceuticals they prescribe, and increase the efficiency of the drug therapies that are needed.
References:
- Tan, A., Wang, M., Liu, J., Huang, K., Dai, D., Li, L., Shi, H., & Wang, P. (2020). Efficacy and safety of acupuncture combined with western medicine for anxiety: A systematic review protocol. Medicine, 99(31), e21445. https://doi.org/10.1097/MD.0000000000021445
- NIH (2015). Acupuncture: in Depth. NIH, National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/acupuncture-in-depth
- Schweiger, V., Secchettin, E., Castellani, C., Martini, A., Mazzocchi, E., Picelli, A., Polati, E., Donadello, K., Valenti, M. T., & Dalle Carbonare, L. (2020). Comparison between Acupuncture and Nutraceutical Treatment with Migratens® in Patients with Fibromyalgia Syndrome: A Prospective Randomized Clinical Trial. Nutrients, 12(3), 821. https://doi.org/10.3390/nu12030821
- Wikipedia (2022). Acupuncture. Wikipedia. https://en.wikipedia.org/wiki/Acupuncture
- Anna Zajacova, Hanna Grol-Prokopczyk, Zachary Zimmer; Pain Trends Among American Adults, 2002–2018: Patterns, Disparities, and Correlates. Demography 1 April 2021; 58 (2): 711–738. doi: https://doi.org/10.1215/00703370-8977691
- Brigham and Women’s Hospital. (2021). One in five American adults experience chronic pain. ScienceDaily. Retrieved July 11, 2022 from www.sciencedaily.com/releases/2021/04/210420092901.htm
- NIH (2021). Opioid Overdose Crisis. NIH, National Institute on Drug Abuse. https://nida.nih.gov/research-topics/opioids/opioid-overdose-crisis
- Searing, Linda (2022). Acupuncture could reduce tension headaches by half. The Washington Post. https://www.washingtonpost.com/health/2022/07/05/acupuncture-eases-tension-headaches/
- Schweiger, V., Secchettin, E., Castellani, C., Martini, A., Mazzocchi, E., Picelli, A., Polati, E., et al. (2020). Comparison between Acupuncture and Nutraceutical Treatment with Migratens® in Patients with Fibromyalgia Syndrome: A Prospective Randomized Clinical Trial. Nutrients, 12(3), 821. MDPI AG. Retrieved from http://dx.doi.org/10.3390/nu12030821#
- Whelan, C. (2022). How Acupuncture May Relieve Symptoms of Multiple Sclerosis. Healthline. https://www.healthline.com/health/managing-ms/acupuncture-for-ms
- Dooley Young (2020). Medicare Opts to Cover Acupuncture for Pain Amid Opioid Crisis. Medscape. https://www.medscape.com/viewarticle/924534?reg=1
- Dahlhamer, J. M., Connor, E. M., Bose, J., Lucas, J. L., & Zelaya, C. E. (2021). Prescription Opioid Use Among Adults With Chronic Pain: United States, 2019. National health statistics reports, (162), 1–9.