Summary
When asked how someone died, ‘they died of old age’ is an acceptable answer – it is given as the cause, like a heart attack, stroke, or cancer. However, unlike these other answers, aging is not classified as a disease. But should it be? This article will discuss the debate over whether aging should be considered a disease, the arguments for and against such a classification, what it would mean from a clinical standpoint, and how it would transform the pharmaceutical and nutraceutical industries.
Figure 1. Is aging the foundation of disease? Is it one by itself? Lifespan.io (n.d.)
As noted in a recent article, aging is not recognized as a ‘disease’ by any country in the world (Bulterijs et al., 2015). However, some researchers, clinicians, and policy experts say that this should change because without the classification of ‘biological disease’ it is difficult to conduct human clinical trials, gain regulatory approval and bring aging therapies to market. Proponents of reclassifying aging point to the “geroscience hypothesis”, which suggests that aging is the number one risk for all chronic diseases, and thus, when trying to improve the number of years humans’ live healthy lives (increasing healthspan) we should focus on treating aging rather than each chronic condition at a time (Tournas & Marchant, 2019). But, the scientific community is not in agreement, as some fear that formally classifying aging as a disease could have a detrimental effect on elderly care.
Reasons for classifying aging as disease:
The debate over whether or not aging should be classified as a disease has gone on for thousands of years, but modern science has allowed us to gain insight into the biological mechanisms behind aging – i.e. cellular senescence [Figure 2]. Senescent cells are cells which have stopped dividing, but don’t die off, and their accumulate results in many of the changes that are considered hallmarks of aging and age-related disease (Wrinkles in skin, and the calcification of blood vessels in the heart – i.e. cardiovascular disease) (Faragher & Calimport, 2019; Childs et al., 2017).
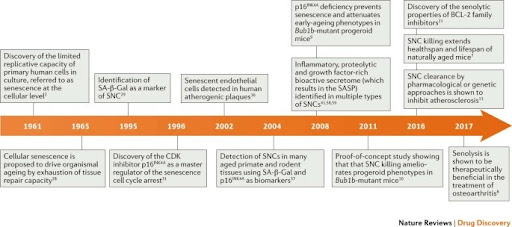
Figure 2. Timeline of understanding cellular senesce and applying it to therapeutic development (Childs et al., 2017).
While research into cellular senescence (and other areas of aging) has promise in regards to developing therapeutics, without the formal classification of ‘disease’, there is no pathway to market for a drug which mitigate the cellular processes underlying aging (Renstrom, 2020). A formal classification would also encourage more funding to be allocated to aging research.
In fact, an international group of researchers specified how crucial a disease classification is in order for aging to receive the necessary allotment of resources at an infrastructure-level. In their publication, these researchers called for the classification of ‘organismal senescence and aging-related diseases’ in 2019, ahead of the revision of the World Health Organization’s International Classification of Disease (ICD). They stressed that this debate is not about a label, but about creating a comprehensive public-health response to aging (conducting clinical trials, giving diagnoses, and prescribing and administering treatment).
While the assembly did not follow the advice of the previously discussed group of researchers to formally recognize aging as a disease, the WHO took a middle-ground approach by implementing an extension code for ‘Aging-related’ (XT9T) diseases (defined as: diseases “caused by pathological processes which persistently lead to the loss of organism’s adaptation and progress in older ages”) (WHO, 2019). The ICD began in the 19th century and is regularly updated, the latest revision of it, the ICD-11, was adopted by the 72nd World Health Assembly and will come into effect on 1st January 2022 (WHO, 2019). The inclusion of an extension code for aging is an encouraging step for proponents of formally classifying aging as a disease, as it signals a shift in the willingness of institutions to put their weight behind such a recognition.
How it would affect Clinical treatment/ medical professionals
The USA has a rapidly aging population, and it is going to put a strain, both on the country’s health-care system, and its economy. The <65 population is expected to rise from 57 million people today (in 2021) to over 80 million people by 2050 (Grunebau,, 2021). This demographic faces living more years with a disability – by 2065 the number of Americans needing long-term care services for help with activities like bathing and eating will double from 7 to over 14 million [Figure 3]. And, the explosive need for long-term care means more spending – men who turn 65 in the next few years will spend ~$142,000, whereas women will spend ~$176,000.
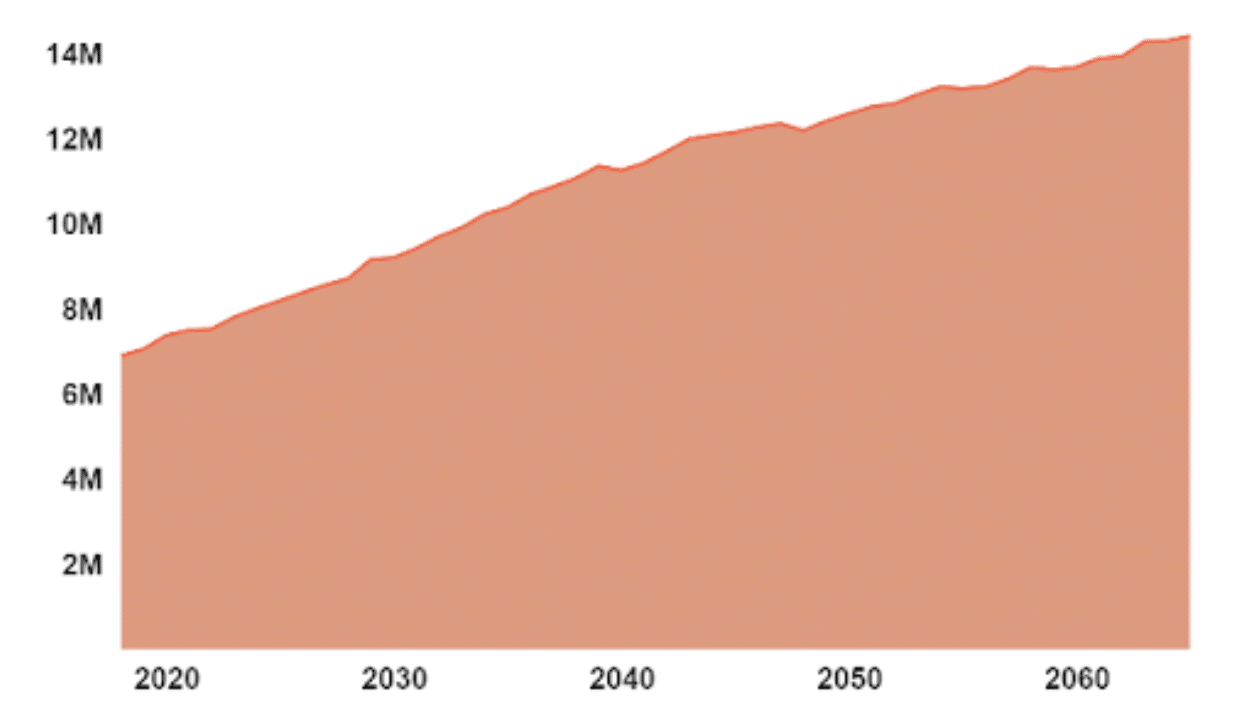
Figure 3. Long-term Care Users in the USA (millions) (Grunebau,, 2021).
Thus, just looking at treatment which mitigates age and aging-related diseases from an economical standpoint, the impact it could have is enormous. In fact, researchers used a ‘value of statistical life” model, and found that just 2.6 more years of ‘healthy living’ could result in a $83 trillion value to the economy (Critchfield, 2021).
Moreover, the amount of non-healthy old people will greatly impact the health-care industry, as doctors, nurses, and long-term care facilities will have to adapt (and in many cases scramble) to try to keep up with the increased demand. This is one of Dr. David Sinclair’s primary arguments in support of classifying aging as a disease; he says that, in the USA we don’t practice medicine, but instead “we’re practicing sick care – or what I call ‘whack-a-mole medicine” (Critchfield, 2021). Dr. Sinclair, who is a professor of genetics and co-director of the Paul F. Glenn Center for Biology of Aging Research at Harvard Medical School, recommends that to relieve the medical community of this influx in patients, we should work on “targeting aging itself” (Critchfield, 2021).
How it would affect Pharmaceutical & Nutraceutical industries
Already, the greater acceptance of aging as a disease is benefiting the pharmaceutical and nutraceutical industries: ICD codes are a prerequisite for the registration of all new drugs and therapies, and the public is increasingly receptive to products whose health claims connect lifespan and healthspan. Thus, the WHO’s inclusion of the extension code for aging-related diseases in the latest ICD will help overcome the “regulatory obstacles that have thus hampered the development of therapeutic interventions and preventative strategies targeting aging and age-related disease” (The Lancet Diabetes Endocrinology, 2018).
Reasons against classifying aging as disease
There are experts, such as Dr. Suresh Rattan of Denmark’s Aarhus University’s Laboratory of Cellular Ageing who believes that, by definition, a condition which everyone experiences cannot be a disease (Renstrom, 2020). On this side of the debate, researchers and industry insiders argue that while aging is a universal experience, it is also a very variable one: there is enormous phenotypical inter-individuality that occurs as we age (i.e. everyone ages differently, and this can be seen both at a cellular and a behavioural level. Consequently, any treatment for aging must span a broad array of symptoms, and lumping them all together under the umbrella of ‘aging’ may be misleading) (The Lancet Diabetes Endocrinology, 2018).
Furthermore, there is concern that classifying aging as a disease might actually be detrimental to older adults: their care could worsen as there would be less of an emphasis to investigate other possible causal factors for any symptoms they may experience. And, from an economics point of view, formally classifying aging as a disease could put older adults at a socio-economic disadvantage as they will have an inevitable disease. This is particularly concerning as ageism already exists in the health-care industry (for instance, many medical practices do not take patients who are on medicare).
Lastly, critics of classifying aging as a disease have raised the alarm over the ability for companies to produce products which play into the ‘aging is a disease’ narrative. These critics say that since there are no currently available drugs or treatments specifically for aging that any products which claim to have these benefits are intentionally misleading; and that this could have serious repercussions in the future, as it makes it difficult for the general public to differentiate between marketing language and scientific research.
Conclusion
Recently, research from Dr. Sinclair and others have shown promise in treating aging as a degenerative process. For example, operating under the theory that aging is caused by the accumulation of epigenetic noise that disrupts gene expression patterns and leads to decreases in tissue function and regenerative capacity – researchers showed that they could restore the vision of aged mice using ectopic expression of OSK transcription factors (Lu, et al. 2020). This experiment is notable as it presents a strong case for the argument that old age is a pathology like any other, and thus, treatable.
There are also advances in human clinical trials, such as the work being done in Dr Sinclair’s lab which is testing novel molecules which raise nicotinamide adenine dinucleotide (NAD+), as NAD levels have been found to decline with age (The Sinclair Lab, 2021).
While this research has exciting potential, in moving forward the biomedical field should remain cognizant of the ability for it to cause real-world consequences to the care and financial standing of older adults. This being said, some researchers have pointed out that the development and marketing of healthspan supplements have already begun, and that it is safer if the FDA is proactive, making this new market fully regulated (Tournas & Marchant, 2019). And hopefully, by legitimizing research into aging as a disease, more effective therapies will be discovered.
References
- Lu, Y., Brommer, B., Tian, X. et al. Reprogramming to recover youthful epigenetic information and restore vision. Nature 588, 124-129 (2020). https://doi.org/10.1038/s41586-020-2975-4
- Faragher, R. & Calimport, S. (2019). Why ageing should be classified as a disease. The Conversation. https://theconversation.com/why-ageing-should-be-classified-as-a-disease-126642
- Childs, B., Gluscevic, M., Baker, D. et al. Senescent cells: an emerging target for diseases of ageing. Nat Rev Drug Discov 16, 718-735 (2017). https://doi.org/10.1038/nrd.2017.116
- Renstrom, J. (2020). Is Aging a Disease? Slate Group : Future Tense. https://slate.com/technology/2020/03/aging-disease-classification.html
- WHO (2019). International Statistical Classification of Diseases and Related Health Problems (ICD), World Health Organization Website https://www.who.int/classifications/classification-of-diseases
- The Lancet Diabetes Endocrinology (2018). Opening the door to treating ageing as a disease. The lancet. Diabetes & endocrinology, 6(8), 587. https://doi.org/10.1016/S2213-8587(18)30214-6
- Critchfield, H. (2021).Is aging a disease? Treating it like one could be worth trillions, study says. Tampa Bay Times. https://www.tampabay.com/life-culture/2021/07/13/is-aging-a-disease-treating-it-like-one-could-save-us-trillions-study-says/
- Grunebaum, D. (2021). How Much Long-Term Care Will YOU Need? MedicareGuide. https://medicareguide.com/how-much-long-term-care-will-you-need-337811
- The Sinclair Lab (2021). Research. Harvard Medical School, https://sinclair.hms.harvard.edu/research
- Lifespan.io (n.d.). What is aging? Lifespan.io, https://www.lifespan.io/aging-explained/



